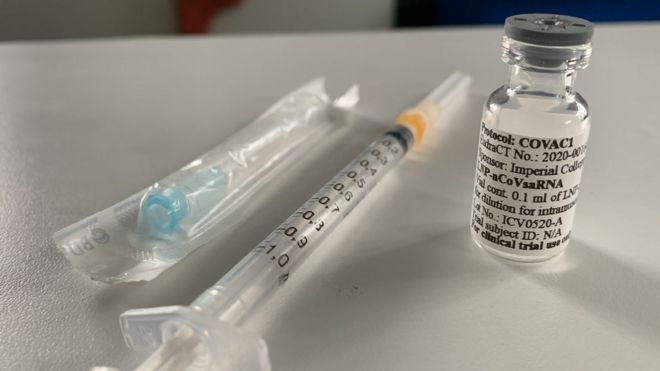
Kuala Lumpur, Malaysia, 24 Feb (Lim Chee Han) – Public excitement prevailed at the arrival of the first batch of COVID-19 Pfizer-BioNTech vaccine in Malaysia on Sunday, probably more as a sign of relief and hope for ending the pandemic soon. Some 312,390 doses of vaccine were reportedly received, and the National COVID-19 Immunisation Programme will be kicked off in phases from 26 February with Prime Minister Muhyiddin Yassin due to receive his first dose under public scrutiny.
The challenge has just begun, aiming to vaccinate more than 80% (more than 26 million) of the population residing in Malaysia within a year, with the first shipment of doses representing merely 0.6% of the doses required (all except one vaccine candidate in the Malaysian vaccine basket requires two doses).
The world is not equal, worse during the pandemic. More than 80% of the population were immunized in Israel by February 18, about the target our government sets for our own country, albeit one year earlier.
Globally, as of February 20, more than 199 million doses have been administered, with 87 countries (45% of the 195 in the world) having received their first vaccines, before Malaysia officially gets its very first dose.
The current projections for global vaccine roll-out suggest that many will have to wait at least three – and up to five – years to cover 75% of the population with a two-dose vaccine, leaving many low-income countries behind.
Due to the growing inequality among countries during the pandemic, the global economy will get hit hard through supply chain disruptions and travel restrictions; the economic impacts are estimated to cost around US$9.2 trillion (RM 36.8 trillion).
Developed economies would pay, too, shouldering half of the burden of the hefty cost, if they let poorer countries go un-vaccinated for longer periods.
Given that the acute global demand for vaccines far outstrips the current production capacity and supply from a limited number of manufacturers, “vaccine nationalism” exacerbates the global inequality.
The world map of vaccine contracts shows exactly that: a small group of wealthy nations has procured the bulk of the global vaccine supply, reserved more than enough vaccine doses for their own domestic use (e.g, the UK 3.4x, Canada 3.35x and the European Union 2.3x).
Out of the 9.59 billion doses booked by February 12, if redistributed evenly, that would be enough to cover more than half the world’s population.
Such “vaccine nationalism” coupled with limited manufacturing has caused an “artificial scarcity” that prevents vaccines being shared equitably among countries.
The shortage is not only in vaccines; some countries also find it difficult to obtain adequate COVID-19 related medical products, such as personal protection equipment (PPE), diagnostics, medicines and other medical devices like ventilators.
Artificial scarcity and high demand for such products create a situation where the goods go to places where they can be sold at higher prices, thus resulting in some medical products priced out of affordability at adequate quantity for low-income countries.
Intellectual property (IP), such as patent, trade secret, industrial design and copyright, has been identified as a major barrier for competent manufacturers and suppliers all over the world to ramp up the production of COVID- 19 medical products to meet global demand during this period.
Many patent-holding multinational corporations have shown insufficient plans, lack of willingness or no plans at all to openly license or transfer technologies to competent manufacturers globally.
Even if some of the corporations did offer voluntary licences, they set the conditions for their chosen partners to determine where to supply and at what price.
At the beginning of the pandemic, American bio-pharmaceutical company Gilead Sciences already set a negative precedent: excluding nearly half of the world’s population (including Malaysia) from accessing alternative suppliers at a lower price for an early potential COVID-19 drug treatment (remdesivir), which has now been de-listed by the WHO for lack of efficacy.
Plenty of evidence has shown that the IP barrier to access to medical products and tools is real. Malaysia is vulnerable to such patent-barrier-induced medical products shortage.
Malaysian-owned patents comprise only 4% out of the total number of patents granted for pharmaceutical products in Malaysia from 2003-2018.
The top 10 foreign countries whose companies and other entities took control of nearly 80% of all pharmaceutical patents in Malaysia were the US, Switzerland, Germany, Japan, France, the UK, Belgium, Sweden, Italy and South Korea.
This corresponds to 56.1% share or RM 22.8 billion worth of all pharmaceutical imports from these 10 countries alone for the past five years (2016-2020).
This shows the degree of high dependency Malaysia has on imported medical products, given that the trade deficit in the pharmaceutical sector is widening year-to-year to the tune of RM 1.06 billion in 2020.
What is more concerning is that the pharmaceutical imports for 2020 dipped significantly by 18.6% compared to the preceding year.
Perhaps this is caused by pandemic-driven supply chain disruptions and global shortages (due to acute high demand).
Given these circumstances, South Africa and India put forward a proposal to the TRIPS Council at the World Trade Organization (WTO) on October 2, 2020, requesting a temporary waiver to be granted to WTO members so that they do not have to implement, apply or enforce certain IP obligations related to COVID-19 products and technologies for a certain period of the pandemic.
The TRIPS Agreement requires all WTO members to grant 20 years of patent monopoly for products (including medical products) if they satisfy certain criteria and conditions.
This “waiver proposal” that now has support of nearly 100 member countries would empower countries to do their best within their policy space to scale up manufacturing capacity, engage in R&D collaboration to develop new treatment and tools, allow transfer of technology, and have access to the increased supply of COVID-19 products and tools from other competent manufacturers, without the fear of expensive litigation.
This proposal would be also useful to provide expedited legal certainty and clarity to the competent manufacturers, especially those in developing countries like Malaysia, to effectively leverage their un-utilised capacity or invest in new capacity to ensure sufficient and affordable global supply of such life-saving products.
Given the glaring global failure of fair distribution of COVID-19 related resources, some countries have come into the painful realisation that relying on the mercy and limited voluntary actions from the pharmaceutical corporations is perhaps not the solution in a global pandemic.
While a growing number of countries have voiced their support for the waiver proposal (with the co-sponsors now including the entire group of African countries and a few others in addition to South Africa and India), not surprisingly, the opposition to the proposal mainly consists of the top patent-holding developed countries including the US, the UK, Japan, the EU, and Switzerland.
This pandemic is unprecedented in human history in terms of the number of people infected and who have died from the disease.
So, delivering universal, affordable and timely access to vaccines and critically important medical treatments should not be left to monopolistic market forces.
In fact, several corporations have received enormous amounts of public funding and investment supporting the COVID-19 R&D.
Moreover, governments, health care workers, patients, and healthy volunteers have also contributed substantially to clinical trials and other scientific research to advance the knowledge and significantly enhance the R&D activities on different therapeutics and vaccines.
Therefore, it is completely legitimate to ask for COVID-19-related IP to not be enforced during this pandemic period.
The current flexibilities in the TRIPS Agreement, including government issuance of compulsory licence, is a piecemeal solution at best and would not provide timely responses during the global health emergency for the government to obtain the necessary access to COVID-19 products, treatments and vaccines.
Thus, it is high time for all governments to unconditionally support the waiver proposal that has already garnered the support of more than 100 countries at the WTO.
It is the right thing to do for each country (especially if we all care to get our vaccine shots as soon as possible), and everyone in the world will benefit from it.
Published in SUNS #9292 dated 24 February 2021